|
Contraindications to internal jugular venous access include severe coagulopathy, the presence of another device at the site, and altered local anatomy, especially if there is a concern for thrombosis from initial catheter placement. It is often the preferred site of access for CVL placement. Right internal jugular venous access allows a straight and direct path to the superior vena cava and has a low rate of catheter malposition during placement. As it courses forward, it joins the subclavian vein to form the brachiocephalic (innominate) vein. Here the vein is most superficial, located only 1 to 1.5 cm below the skin surface in most patients. Caudal to the cricoid cartilage, the internal jugular vein can be found between the two heads of the sternocleidomastoid muscle at the base of the neck. As it travels towards the chest, it assumes an anterolateral position to the common carotid artery beneath the sternocleidomastoid muscle. It is contained within the carotid sheath and travels with the carotid artery and the vagus nerve. The internal jugular vein exits the skull base from the jugular foramen collecting blood from the sigmoid sinus. However, when ultrasound guidance is not feasible, CVLs may be placed using anatomical landmarks without ultrasound. Ultrasound guidance can benefit all approaches and is recommended for every CVL placement. The subclavian vein approach is at higher risk for pneumothorax than the internal jugular vein approach. The femoral veins are compressible sites and, as such, may be more appropriate for patients who are at high risk of bleeding. The right internal jugular and subclavian valves are the most direct paths to the right atrium via the superior vena cava. There are three possible sites for CVL placement in adult patients: namely, the internal jugular, femoral, and subclavian. This article will detail the anatomy of the site placement, indications and contraindications, equipment and personnel involved, technique, preparation, and associated complications.  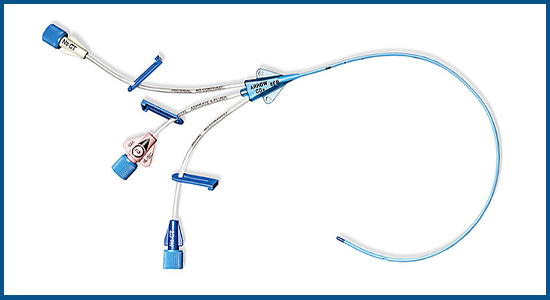
With ultrasound guidance, standardized techniques, new catheter designs, and central line care bundle, this procedure has become ubiquitous in the intensive care unit. Over the past decade, there has been tremendous improvement and reduced complications associated with central line placement procedures. According to epidemiologic data, 8% of hospitalized patients require central venous access, and more than 5 million central venous catheters are inserted in the United States annually. Central line placement is an essential skill, especially in critical care units. Now referred to as the Seldinger technique, this procedure allows the safe and reliable insertion of a central venous catheter in the large lumen central veins. Sven-Ivar Seldinger, in 1953 introduced the method to facilitate catheter placement into the central veins lumens. 
A central venous line (CVL) is a large-bore central venous catheter placed using a sterile technique (unless an urgent clinical scenario prevents sterile technique placement) in specific clinical procedures.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
